Can U Still Get Pregnant Again With a 5 Mm Endometrium Thickness
- Enquiry
- Open Access
- Published:
The correlation between endometrial thickness and pregnancy outcomes in fresh ART cycles with different age groups: a retrospective study
Middle E Fertility Society Journal book 24, Article number:10 (2020) Cite this article
Abstract
Groundwork
In assisted reproductive technology (ART) cycles in improver to embryo quality, the receptivity of the endometrium plays the main role in clinical outcomes. Endometrial receptivity is necessary to implantation of an embryo, and ultrasound has been established every bit an appreciated, simple, and not-invasive technique in the evaluation of the endometrial preparation before embryo transfer in fresh in vitro fertilization (IVF) cycles. Fence on the predictive value measuring endometrial thickness before administering homo chorionic gonadotropin (HCG) for ovulation triggering in ART is ongoing. In order to explore the touch on of endometrial thickness on triggering day on ongoing pregnancy rate (OPR) in Fine art cycles, nosotros retrospectively analyzed information from 1000 patients undergoing IVF/ICSI cycles.
Results
The data showed pregnancy rate was increased in the endometrial thickness of 8 mm to xi mm so decreased, and in endometrial thickness (Ent) > fourteen mm, pregnancy rate was nada. There were pregnant differences in endometrial thickness and pregnancy outcomes between different age groups. The pregnancy rate was higher (32%) in 23–30 years old women, and the range of Ent in this group was six–12 mm. Also, the data showed a positive correlation between Ent with AMH and estradiol levels and the number of COC and MII oocytes and a negative correlation between female age with Ent.
Conclusion
The issue showed that Ent on hCG assistants day is associated with pregnancy outcomes in fresh IVF/ICSI cycles with different age groups, although some of the clinical parameters may have an upshot on Ent. Large studies are needed to make a definitive determination.
Background
Assisted reproductive engineering has been usually used in infertility treatment over the by 3 decades. In improver to embryo quality, the receptivity of the endometrium plays a primary role in clinical effect [1]. Endometrial receptivity is necessary to implantation of an embryo, and ultrasound has been established as an appreciated, simple, and not-invasive technique in evaluation of endometria training before embryo transfer in fresh IVF cycles. Several sonographic parameters have been assessed that include endometrial thickness (Ent), endometrial design (EnP), endometrial book, and sub-endometrial blood menses [2]. Trans-vaginal ultrasonography (TVU) is frequently used to mensurate Ent on the twenty-four hours of HCG administration every bit the best echogenic space between the junction of the endometrium and myometrium in the mid-sagittal plane. It has been widely suggested that a thin endometrium is related to lower IVF–ICSI pregnancy rates, just an agreement is still lacking on what the verbal definition of thin endometrium [3]. Debate on the predictive value measuring Ent before administering HCG for ovulation triggering in assisted reproduction techniques is ongoing. Some of the investigators have shown a linear correlation between pregnancy rates and Ent, though others accept posited that pregnancy rates may even deteriorate above a thickness of 14 mm and then miscarriage rates may increase [4]. In order to explore the impact of endometrial thickness on triggering twenty-four hours on ongoing pregnancy charge per unit (OPR) in IVF–ET cycles, nosotros retrospectively analyzed data from 1000 patients with different age groups undergoing IVF/ICSI cycles.
Methods
The study was a retrospective report and was done by reviewing the clinical data of fresh IVF/ICSI cycles at the Yazd Research and Clinical Centre for infertility from May 2016 until May 2018. The study included women aged eighteen–45 years without endometriosis. Also, patients with severe male person factor infertility, patients with a known endometrial polyp or uterine anomaly, oocyte donation cycles, and preimplantation genetic diagnosis (PGD) cycles were excluded.
Ovarian stimulation
Ovarian stimulation, sperm preparation, IVF embryo culture, and fresh ET protocols in our eye have been described elsewhere [5, 6]. Briefly, according to the maternal age, cause of infertility, ovarian response, and coexisting medical conditions, agonist and antagonist ovarian stimulation protocols were washed [6]. Recombinant human chorionic gonadotropin (hCG) (250 mg; Ovidrel, Serono, Geneva) or urinary HCG (10,000 IU, Pregnyl, Organon, Netherland) was administered to trigger ovulation when ii leading follicles reached a hateful diameter of 17 mm. Trans-vaginal ultrasound-guided oocyte retrieval was conducted 36 later on hCG administration. Fertilization of the oocytes took identify either by IVF or ICSI, according to the sperm quality. The luteal stage was supported past vaginal progesterone (Cyclogest, Actavis, United kingdom), 400 mg, and twice a day. One or ii embryos were transferred two days after. Fertilization charge per unit was defined as the percent of fertilized oocytes (2PN) to all mature oocytes (MII). Chemic pregnancies were confirmed 2 weeks after embryo transfer, past positive serum βHCG measurement. Clinical pregnancy was defined by the presence of gestational sac in the uterus, 4 weeks later on embryo transfer. The implantation rate estimated past the number of gestational sacs that visualized on TVU divided by the number of embryos transferred [6].
Endometrial assessment
Ent was measured by TVU on the day of triggering. In the longitudinal aeroplane of the uterus, the maximum distance between the two interfaces of endometrium–myometrium junction was divers as the thickness of endometrium [7].
Statistical analysis
Results are showed equally the mean ± standard deviation (SD) or percentage (%). The means of samples with normal distribution and of sufficient size were compared by Student's t exam and one-way ANOVA. Differences betwixt aberrant scatterings and the medians were compared past Mann-Whitney U and Kruskal-Wallis test. Chi-square (χ ii) test was employed to assess the differences between categorical variables. A p value < 0.05 was considered meaning. Statistical assay was performed using the Statistical Parcel for the Social Sciences xx (SPSS Inc., Chicago, IL, U.s.).
Results
One thousand fresh IVF/ICSI cycles were recruited in this study, among which 277 cycles achieved chemical pregnancy (27.seven%), and from them, 245 cycles achieved clinical pregnancy (88.iv%).
To explore the relationship betwixt endometrial thickness and chemical and clinical pregnancy rates in all the m cycles, patients were divided into 9 singled-out groups co-ordinate to the endometrial thickness on the twenty-four hour period of embryo transfer: ≤ 7 mm, vii–viii mm, viii–nine mm, ix–10 mm, x–11 mm, 11–12 mm, 12–13 mm, xiii–xiv mm, and ≥ 14 mm. Chemical and clinical pregnancy rates were calculated for each endometrial thickness interval.
There was a significant correlation between Ent and pregnancy outcomes (p < 0.0001). Also, the data testify that by increasing the endometrium thickness to 11 mm, pregnancy increases and and so decreases (Table one, Fig. 1).
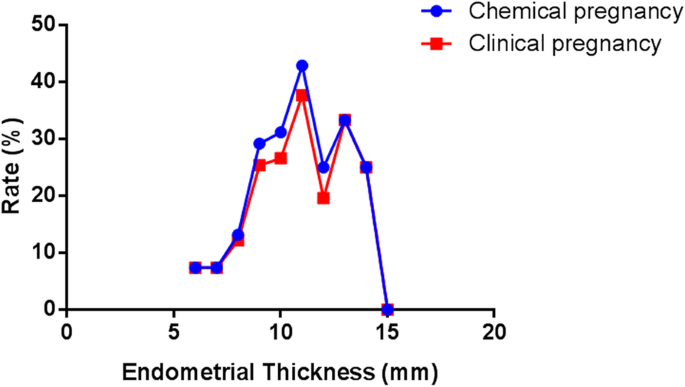
The human relationship between endometrial thickness and pregnancy outcomes
There were significant differences in clinical parameters like female age, AMH, estradiol level on the day of last triggering, and the numbers of retrieved oocytes and oocyte maturity in pregnant patients compared to non-significant (Table ii).
Also, for determining the event of female person historic period on the pregnancy rate and the relationship with endometrial thickness, we divided patients to iv dissimilar age groups: 18–23, 23–xxx, 30–38, and > 38. The data showed the charge per unit of pregnancy was significantly different between dissimilar historic period groups (p = 0.001), and in group two were higher than others. Also, when nosotros compared endometrial thickness between different age groups, nosotros saw that the range of Ent in group two was 6–12 mm that confirms our results in Table ane(Tables iii and 4).
The information showed a positive correlation betwixt Ent with AMH and estradiol levels and the number of COC and MII oocytes. On the other hand, there is a negative correlation betwixt female age and Ent (Table 5).
Discussion
We had studied fresh IVF/ICSI cycle of 1000 patients and determined the consequence of Ent on the day of last triggering on pregnancy result. Our results showed that at that place is a pregnant correlation between endometrial thickness and pregnancy rate.
While several studies take confirmed the association of thin endometrium with depression clinical pregnancy rate, the Ent cutoff point for IVF–ET pregnancy outcome has not been identified. Studies showed that the clinical pregnancy rate and ongoing pregnancy rate are significantly reduced when Ent is less than 7 mm on the hCG day [7, eight] that was in line with our study. Information technology was reported that spontaneous ballgame rate is significantly increased when Ent > xiv mm [9], whereas another report proposes at that place is no adverse upshot on pregnancy outcome when Ent > 14 mm [7]. In our study, we observed that pregnancy rate was increased from Ent = 8 mm to Ent = eleven mm, then decreased, and in Ent > 14 mm, the pregnancy charge per unit was null.
In order to get a more accurate relationship between endometrial thickness and IVF upshot, Bu et al. demonstrated that for the patient undergoing IVF with the different ovarian response, a thin endometrial thickness on HCG assistants twenty-four hours is associated with lower pregnancy charge per unit [10]. A thick endometrium is more than controversial. Several previous investigators have suggested that a thick endometrium (> 16, or ≥ 17 mm) is associated with an improved conception rate, whereas others have reported a detrimental outcome of a thick endometrium (> 14 mm) on formulation rate [11, 12]. Yuan et al., in their study, plant a consistently positive correlation between Ent and conception rate, with patients having an Ent greater than 15 mm achieving the highest conception charge per unit of 53.3% [3]. It is important to note, still, that a thickened endometrium is associated with a number of intrauterine pathologies such as polyps or fibroids, both of which accept been shown to adversely affect implantation and reduce pregnancy rates [13]. Therefore, in women with an abnormally thickened endometrium, it seems prudent to bear out farther investigations, such as a hysteroscopy to rule out and treat whatever intra-cavity lesions.
Vânia Costa Ribera and coworker in a report evaluated whether Ent affects the issue of a fresh embryo transfer, in a retrospective, single-heart accomplice of 3350 IVF cycles. In the multivariate regression analysis, Ent was not-linearly associated with alive nascence, live birth rates being the lowest with an Ent less than seven.0 mm (21.6%; p < 0.001) and then between vii.0 and ix.0 mm (xxx.2%; p = 0.008). An Ent less than 7.0 mm was besides associated with a subtract in neonatal birth weight z-scores. They concluded that the use of Ent is a potential prognostic tool for live nativity rates and neonatal birth weight [iv].
Mohammady and coworker in their study evaluated the issue of combined endometrial thickness and design on the success of intracytoplasmic sperm injection (ICSI) cycles and concluded endometrial thickness of 10–12.9 mm with trilaminar design is associated with higher CPR with ICSI cycles [14].
Julian et al. in their study evaluated the effect of endometrial pattern at triggering twenty-four hour period on implantation [15]. The endometrial pattern (Enp) was recorded as being in i of the following three categories, as described past Grunfeld et al. [xvi]: (i) belatedly proliferative (hyperechoic endometrium constituting < 50% of the Ent, with a hyperechoic basalis and hypoechoic functional), (two) early secretory (hyperechoic basalis and functional extending to > 50% of the Ent, but not roofing the entire endometrial cavity), and (3) mid-late secretory (homogeneous hyperechoic functionalize extending from the basalis to the lumen). Within the study population, Ent was not significantly associated with clinical outcomes of euploid ETs. A type three Enp at trigger twenty-four hours suggests a prematurely airtight window of implantation [15].
Zhao and coworker showed a significant difference in endometrial thickness on the 24-hour interval of HCG administration and the change in endometrial thickness from the third twenty-four hour period of gonadotropin stimulation to the mean solar day of HCG administration between meaning women and not-pregnant women. This finding indicates that adequate endometrial development is favorable for improved pregnancy rate. They propose that the endometrium of non-pregnant women may be associated with pathological abnormalities, such every bit squamous cell metaplasia or lacking a normal proliferative response to the rising estradiol level. In a binary logistic regression model, the endometrial thickness on day 3 of gonadotropin stimulation, endometrial thickness on the twenty-four hours of HCG administration, and the change in endometrial thickness from the third day of gonadotropin stimulation to the day of HCG administration were independent predictive factors for pregnancy [1] Although many studies have evaluated the relationship between endometrial thickness and IVF outcome, the results are all the same controversial. Some authors reported no relationship between endometrial thickness and pregnancy charge per unit in patients undergoing IVF [17, 18].
Because of patient basic parameters, such as the number of oocytes retrieved, quality and the number of embryos transferred were not fine assessed in nigh studies, and the results from them were questionable. In our study, we showed that there is a significant difference between clinical parameters like AMH, estradiol level on the day of concluding triggering, and the numbers of retrieved oocytes and mature oocytes in the pregnant and non-pregnant patients. As well, there was a positive correlation betwixt Ent with these clinical parameters. Ent is a crucial factor for pregnancy, but in that location is a possibility that these parameters may be more of import than Ent and may have an effect on it. In fact, ovarian reserve and internal estradiol production cause endometrial growth. AMH is considered a sign of the ovarian reserve; for instance, it is generally expressed by those follicles that are newly progressive from the primordial follicle pool. Hence, serum AMH levels are demonstrative of the number and feature of the ovarian follicular pool [19]. Besides, AMH is related to the number of mature oocytes and fertilization rates. On the other hand, there was a negative correlation between Ent and female person age. We plant that female age is an of import factor in fertility, and its increase, although negligibly, leads to a reduction in the clinical pregnancy charge per unit. Keane et al. in line with our study showed that both AFC and AMH are strongly dependent on patient age and can estimate IVF outcomes, including pregnancy and alive nativity rates [twenty]. Reichman and colleagues showed that AMH is a properly strong metric for the prediction of Fine art cancelation and how many oocytes may be retrieved after stimulation, but conversely, they showed it was a moderately poor exam for the prediction of pregnancy later on whatever given treatment cycle. Patients with extremely low levels of AMH still can attain reasonable handling outcomes and should not exist precluded from attempting IVF solely on the ground of an AMH value [21]. Studies showed that an increasing number of full oocytes, zygotes, and the quality of embryos are associated with live nascence following donor oocyte IVF cycles [10, 22]. Barton et al. found that historic period and E2 on the solar day of hCG assistants were predictive of mature oocytes and embryos retrieved, only FSH was non [23].
Conclusion
Our study demonstrated that Ent in hCG administration twenty-four hours correlated with pregnancy outcomes in fresh IVF/ICSI cycles. The highest pregnancy rate was accompanied by viii–xi mm endometrial thicknesses and decreased to nil when Ent was > 14 mm. Also, there was a positive correlation between Ent and clinical parameters and tin can bear on pregnancy outcomes. On the other hand, we institute the female age had a negative correlation with Ent and pregnancy outcomes.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the respective writer on reasonable request.
Abbreviations
- AMH:
-
Anti-Mullerian hormone
- Fine art:
-
Assisted reproductive engineering
- CPR:
-
Clinical pregnancy rate
- EnP:
-
Endometrial blueprint
- Ent:
-
Endometrial thickness
- ET:
-
Embryo transfer
- HCG:
-
Human chorionic gonadotropin
- ICSI:
-
Intracytoplasmic sperm injection
- IVF:
-
In vitro fertilization
- OPR:
-
Ongoing pregnancy rate
- TVU:
-
Trans-vaginal ultrasonography
References
-
Zhao J, Zhang Q, Wang Y, Li Y (2014) Endometrial pattern, thickness and growth in predicting pregnancy result post-obit 3319 IVF cycle. Reprod BioMed Online 29(three):291–298
-
Kader MA, Abdelmeged A, Mahran A, Samra MFA, Bahaa H (2016) The usefulness of endometrial thickness, morphology and vasculature by 2d Doppler ultrasound in prediction of pregnancy in IVF/ICSI cycles. Egypt J Radiol Nucl Med 47(1):341–346
-
Yuan X, Saravelos SH, Wang Q, Xu Y, Li T-C, Zhou C (2016) Endometrial thickness as a predictor of pregnancy outcomes in 10787 fresh IVF–ICSI cycles. Reprod BioMed Online 33(2):197–205
-
Ribeiro VC, Santos-Ribeiro Due south, De Munck North, Drakopoulos P, Polyzos NP, Schutyser V et al (2018) Should nosotros continue to measure endometrial thickness in modern-mean solar day medicine? The effect on live nascence rates and birth weight. Reprod BioMed Online 36(4):416–426
-
Eftekhar M, Firouzabadi RD, Karimi H, Rahmani E (2012) Outcome of cryopreserved-thawed embryo transfer in the GnRH agonist versus antagonist protocol. Iran J Reprod Med ten(iv):297
-
Eftekhar Thousand, Mohammadian F, Yousefnejad F, Khani P (2013) Microdose GnRH agonist burst versus ultrashort GnRH agonist combined with fixed GnRH antagonist in poor responders of assisted reproductive techniques cycles. Int J Fertil Steril 6(4):266
-
Fang R, Cai L, Xiong F, Chen J, Yang W, Zhao X (2016) The issue of endometrial thickness on the 24-hour interval of hCG administration on pregnancy outcome in the first fresh IVF/ICSI cycle. Gynecol Endocrinol 32(vi):473–476
-
Eftekhar G, Tabibnejad N, Tabatabaie AA (2017) The thin endometrium in assisted reproductive technology: an ongoing challenge. Middle Due east Fertil Soc J 23(1):1–7
-
Weissman A, Gotlieb 50, Casper RF (1999) The detrimental effect of increased endometrial thickness on implantation and pregnancy rates and effect in an in vitro fertilization program. Fertil Steril 71(i):147–149
-
Bu Z, Sun Y (2015) The impact of endometrial thickness on the mean solar day of human chorionic gonadotrophin (hCG) administration on ongoing pregnancy charge per unit in patients with different ovarian response. PLoS I ten(12):e0145703
-
Al-Ghamdi A, Coskun South, Al-Hassan S, Al-Rejjal R, Awartani K (2008) The correlation between endometrial thickness and result of in vitro fertilization and embryo transfer (IVF-ET) outcome. Reprod Biol Endocrinol 6(1):37
-
Richter KS, Bugge KR, Bromer JG, Levy MJ (2007) Relationship between endometrial thickness and embryo implantation, based on one,294 cycles of in vitro fertilization with transfer of two blastocyst-stage embryos. Fertil Steril 87(1):53–59
-
Pritts EA, Parker WH, Olive DL (2009) Fibroids and infertility: an updated systematic review of the evidence. Fertil Steril 91(4):1215–1223
-
Al Mohammady M, Fattah GA, Mahmoud M (2013) The impact of combined endometrial thickness and design on the success of intracytoplasmic sperm injection (ICSI) cycles. Heart East Fertil Soc J 18(3):165–170
-
Gingold JA, Lee JA, Rodriguez-Purata J, Whitehouse MC, Sandler B, Grunfeld Fifty et al (2015) Endometrial pattern, merely not endometrial thickness, affects implantation rates in euploid embryo transfers. Fertil Steril 104(iii):620–viii. e5
-
Grunfeld L, Walker B, Bergh PA, Sandler B, Hofmann G, Navot D (1991) High-resolution endovaginal ultrasonography of the endometrium: a noninvasive test for endometrial adequacy. Obstet Gynecol 78(2):200–204
-
Bassil S (2001) Changes in endometrial thickness, width, length and pattern in predicting pregnancy effect during ovarian stimulation in in vitro fertilization. Ultrasound Obstet Gynecol eighteen(three):258–263
-
De Geyter C, Schmitter Yard, De Geyter M, Nieschlag E, Holzgreve W, Schneider HP (2000) Prospective evaluation of the ultrasound appearance of the endometrium in a cohort of ane,186 infertile women. Fertil Steril 73(1):106–113
-
Peluso C, Fonseca FL, Rodart IF, Cavalcanti Five, Gastaldo G, Christofolini DM et al (2014) AMH: an ovarian reserve biomarker in assisted reproduction. Clin Chim Acta 437:175–182. https://doi.org/10.1016/j.cca.2014.07.029
-
Keane K, Cruzat VF, Wagle S, Chaudhary N, Newsholme P, Yovich J (2017) Specific ranges of anti-Mullerian hormone and antral follicle count correlate to provide a prognostic indicator for IVF event. Reprod Biol 17(1):51–59. https://doi.org/10.1016/j.repbio.2016.12.002
-
Reichman DE, Goldschlag D, Rosenwaks Z (2014) Value of antimullerian hormone as a prognostic indicator of in vitro fertilization outcome. Fertil Steril 101(4):1012–eight e1. https://doi.org/ten.1016/j.fertnstert.2013.12.039
-
Hariton E, Kim Thousand, Mumford SL, Palmor M, Bortoletto P, Cardozo ER et al (2017) Total number of oocytes and zygotes are predictive of alive birth pregnancy in fresh donor oocyte in vitro fertilization cycles. Fertil Steril 108(2):262–268. https://doi.org/ten.1016/j.fertnstert.2017.05.021
-
Barton SE, Missmer SA, Ashby RK, Ginsburg ES (2010) Multivariate analysis of the association between oocyte donor characteristics, including basal follicle stimulating hormone (FSH) and age, and IVF cycle outcomes. Fertil Steril 94(4):1292–1295. https://doi.org/10.1016/j.fertnstert.2009.07.1672
Acknowledgements
Non applicative
Writer information
Affiliations
Contributions
ME, SZ, and BM designed the study and contributed to the acquisition of information. FT and EM analyzed and interpreted the information. ME and EM were the main persons in writing the manuscript. All authors read and approved the final manuscript.
Respective author
Ideals declarations
Ethics approval and consent to participate
The written report was approved past the Scientific and Ideals Committee of Islamic Azad Academy, Yazd Branch, Yazd, Iran (IR. SSU.MEDICINE.REC.1394.338).
Consent for publication
Non applicable
Competing interests
The authors declare that they accept no competing interests.
Boosted data
Publisher'southward Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed nether the terms of the Creative Commons Attribution four.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted utilise, distribution, and reproduction in whatsoever medium, provided you lot give advisable credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Reprints and Permissions
About this article
Cite this article
Eftekhar, Chiliad., Mehrjardi, S.Z., Molaei, B. et al. The correlation between endometrial thickness and pregnancy outcomes in fresh Fine art cycles with unlike age groups: a retrospective study. Middle East Fertil Soc J 24, x (2020). https://doi.org/10.1186/s43043-019-0013-y
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1186/s43043-019-0013-y
Keywords
- Endometrial thickness
- ART
- Female historic period
- Pregnancy
Source: https://mefj.springeropen.com/articles/10.1186/s43043-019-0013-y
0 Response to "Can U Still Get Pregnant Again With a 5 Mm Endometrium Thickness"
Publicar un comentario